02 Feb Living with Locked-in Syndrome
Locked-in Syndrome (LiS) is a rare neurological disorder usually resulting from a lesion to a region of the brainstem called the pons. It can also be caused by a stroke, tumours, infections, certain nerve disorders, or amyotrophic lateral sclerosis (ALS). It acquired its name because patients lose most or all of their motor function, facial control, breathing, swallowing and speaking abilities. However, consciousness and cortical functions are preserved. Tracey Gibbs spoke to us about her experience living with locked-in syndrome.
Brain Foundation (BF): How did you become ‘locked-in’?
Tracey Gibbs (TG): When I was 19 years old, I was having trouble for a week or two with severe headaches. This was out of the norm for me, because I simply didn’t get headaches. I told my doctor this but he kept treating me for migraines, even after I went back several times. A friend took me to his own doctor for a second opinion, but it was too late – the unexpected stroke I had been having was too far gone. The doctor sent me straight to the hospital that afternoon, but in the early hours of the next morning, I was found unconscious. After getting an MRI, we were told that I had experienced a brainstem stroke, caused by an abscess on the brainstem pons. It wasn’t until months later, after meeting Professor Ted Freeman, that I knew just how rare my type of stroke was (a non-blood-related stroke).
It has been 28 years now that I have been “living locked-in”.

BF: I understand that there is an initial period of trying rehabilitation to regain some motor function. What was that like, and how have you managed LiS in the long term?
TG: Well, that may be so, but initially I didn’t receive any kind of rehab – I didn’t respond to the usual treatment, so I found myself put into the “too hard basket” for quite some time. It wasn’t until several years later that I was given a new physiotherapist, and she worked with electrical stimulation. She explained all about the device and what it does, and I was very much intrigued. I was so glad when she asked me if I wanted to give it a try – I had a really good feeling about this treatment. After just a few sessions, I was starting to feel a difference in my arms. Just maybe, I had finally found a treatment that actually got a great response from my body. Years went by, and I was still responding well. As slow as the treatment was, it didn’t bother me, considering how long it took to find.
BF: What was the most helpful thing when adjusting to how your life has changed?
TG: I wouldn’t exactly ask ‘what’, but ‘who’. For years, I only had my mum and the staff at Highgate Park. When I had my first stroke, all my friends suddenly disappeared. The only ones who stayed were family friends, and only my mum visited. I have some great new friends now, but my mum is still my main visitor. It has been great to reconnect with a lot of old high school and primary school friends on Facebook. I have also made friends with people from all over the world. I love it! Until 2006, I just had my TV – mum got me hooked on Days Of Our Lives and other daytime TV programmes. Since I was introduced to social media, everything changed. The world was in my room, and I was no longer “alone”.
BF: LiS is quite different to other disorders of consciousness – do people generally understand this?
TG: I can’t really speak for other survivors of LiS, but because I had a brainstem stroke my face was severely paralysed. It was pulled to the left and my body had extremely low tone. I went out a few times, but people would often stare at me. I tried to ignore it, but I couldn’t handle it. So I hid from the world. I believed that if I couldn’t handle the way I looked, then how could the world? It wasn’t until I started to feel muscle activity in my face that I started to go out again.
When we go out now, if they ask my mum or carer what is wrong with me, they often still have a puzzled look on their face – even after seeing us communicate, and having everything explained. I have found people just don’t get it until they have actually tried to communicate with me.
Well, years have passed and I am feeling more and more like myself every day. This feeling might not be visible to others, but one day I hope it will be!
Resources & Support
Thank you so much, Tracey, for sharing your story with us. Living with locked-in syndrome is quite a rare disorder – but it’s one of many ways that brain diseases & injuries continue to affect people. Even after the acute phase has passed, people can be disabled by these conditions. If you develop symptoms of an acute brain injury (i.e. a sudden, extreme headache; weakness or paralysis on one side of your body), please call 000 or go to a hospital immediately.
Research is essential to prevent brain disorders, improve treatments, and help people manage ongoing symptoms. But it’s also important to share these stories so that we can support the patient community and reduce the stigma around disability.
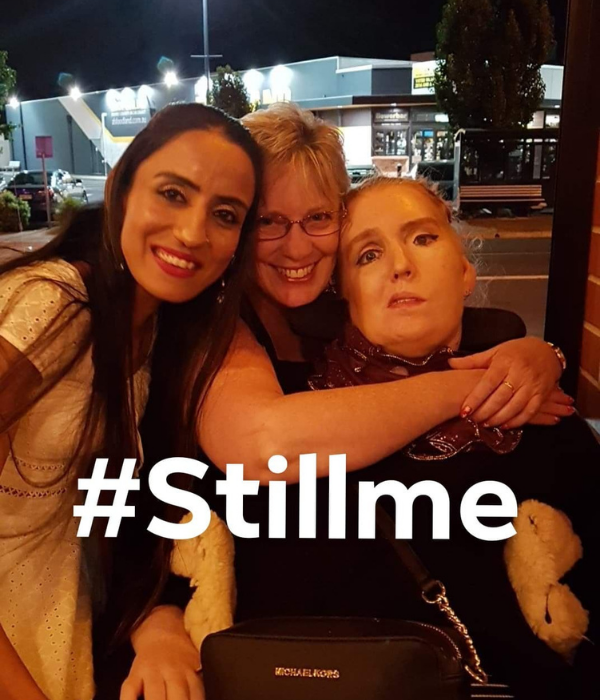
Useful links:
- Locked-In Syndrome – our article about this disorder.
- Tracey’s Facebook page – you can learn more about her story here.
- ARDOC – Australian Register of Disorders of Consciousness. This confidential register helps medical professionals improve care for people with disorders of consciousness (coma, LiS, minimally conscious state, or vegetative state). It also connects the loved ones and carers of the patient via an online forum where they can ask for advice or support.
This interview was first published in our Winter 2021 Brainwaves Newsletter.


 The Brain Foundation is the largest, independent funder of brain and spinal injury research in Australia. We believe research is the pathway to recovery.
The Brain Foundation is the largest, independent funder of brain and spinal injury research in Australia. We believe research is the pathway to recovery.